Search
Showing 1 - 5 of 5 results
 News
News
Inpatient Infusion Therapy for Refractory Headaches: UCSF Case Study
The first center of its kind on the West Coast, the UCSF Headache Center provides patients with comprehensive care to relieve the most debilitating headaches. This includes inpatient treatment for people with severe unremitting or recurring headaches for whom first-line therapies have failed. News
News
Study Finds Paxlovid Treatment Does Not Reduce Risk of Long COVID
A team of researchers from UC San Francisco has found that Paxlovid (Nirmatrelvir-ritonavir) did not reduce the risk of developing long COVID for vaccinated, non-hospitalized individuals during their first COVID-19 infection.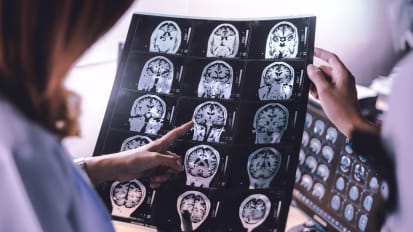 Document
Document
Referral Guide for Physicians - Neurology and Neurological Surgery
Referral and specialty care clinic information provided by UC San Francisco’s departments of Neurology and Neurological Surgery. Document
Document
Headache Center Inpatient Referral Guide
As the only program with an Inpatient Headache Treatment Unit in Northern California, UCSF’s Headache Center helps improve the quality of life for individuals suffering from debilitating headaches.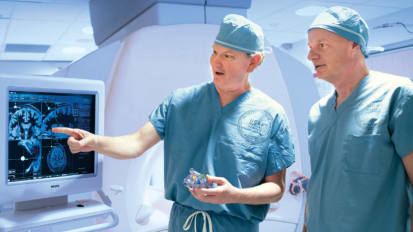 Document
Document
Neurology and Neurological Surgery Services
Our internationally renowned centers, clinics and programs deliver compassionate clinical care while accelerating advances in the diagnosis, treatment and prevention of complex disorders of the brain, spine and peripheral nervous system.

